It has been found that 2.85 billion people around the world lived at risk of infection with Malaria in 2009. India's financial capital Mumbai is reeling with the menace. The city's municipal, government and private hospitals are teeming with malaria patients. Other cities such as Thane, Pune and Nagpur have also reported an alarming number of patients over the past fortnight.
Here's an FAQ on what you need to know about the disease and how you can avoid it.
What is malaria?
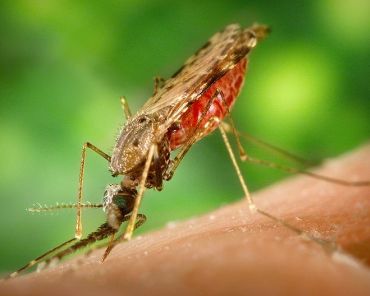
Malaria is caused by a one-celled parasite called a Plasmodium. Female Anopheles mosquitoes pick up the parasite from infected people when they bite them.
Inside the mosquito, the parasites develop and reproduce. When the mosquito bites again, the parasites mix with its saliva and pass into the blood of the person being bitten.
Malaria parasites multiply rapidly in the liver and then in red blood cells of the infected person.
One to two weeks after a person is infected the first symptoms of malaria appear: usually fever, headache, chills and vomiting. If not treated promptly with effective medicines, malaria can kill by infecting and destroying red blood cells and by clogging the capillaries that carry blood to the brain or other vital organs.
There are four types of human malaria: Plasmodium vivax, P malariae, P ovale and P falciparum. P vivax and P falciparum are the most common forms.
...
Courtesy: World Health Organisation
All that you need to know about Malaria
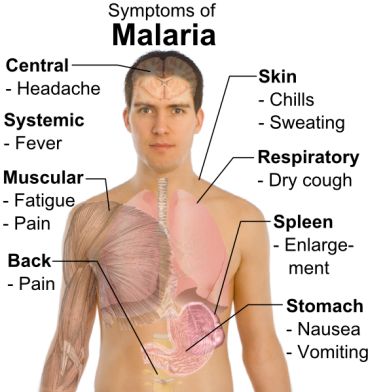
What are the symptoms of Malaria?
Malaria is an acute febrile (sudden onset that manifests with fever) illness. Symptoms appear seven days or more (usually 10 15 days) after the infective mosquito bite.
The first symptoms -- fever, headache, chills and vomiting -- may be mild and difficult to recognise as malaria.
If not treated within 24 hours, P falciparum malaria can progress to severe illness and even lead to death.
Children in endemic areas with severe disease frequently develop one or more of the following syndromic presentations: severe anaemia, respiratory distress in relation to metabolic acidosis, or cerebral malaria. In adults, multi-organ involvement is also frequent.
For both P vivax and P ovale, clinical relapses may occur weeks to months after the first infection, even if the patient has left the malarious area. These new episodes arise from 'dormant' liver forms (absent in P Falciparum and P malariae), and special treatment --targeted at these liver stages -- is mandatory for a complete cure.
The danger signs of severe malaria are:
- Changes in behaviour (convulsions; unconsciousness; drowsiness; confusion; inability to walk, sit, speak, or recognise relatives);
- Repeated vomiting, inability to retain oral medication, inability to eat or drink;
- Passage of small quantities of urine or no urine, or passage of dark urine;
- Severe diarrhoea;
- Unexplained heavy bleeding from nose, gums or other sores;
- Severe dehydration (loose skin and sunken eyes);
- Anaemia and the whites of the eyes turning yellow.
All that you need to know about Malaria
What is the best treatment against malaria? Why combine drugs?
In most parts of the world, Plasmodium falciparum, the most lethal type of human malaria, has become resistant to conventional treatment.
This is the use of a single drug (or monotherapy) of chloroquine, sulfadoxine-pyrimethamine, or another anti-malarial medicine to fight malaria.
World Health Organisation recommends that countries use a combination of anti-malarial medicines to reduce the risk of drug resistance. WHO also recommends combinations that contain derivatives of artemisinin -- a substance extracted from the plant Artemisia annua -- along with another effective anti-malarial drug.
These combinations are called artemisinin-based combination therapies (ACTs). ACTs are currently the most effective treatment for malaria, with a 95 per cent cure rate against falciparum malaria.
Over the past five years, ACTs have been deployed on an increasingly large scale. ACTs produce a rapid clinical cure and are well tolerated by patients. In addition, ACTs have the potential to reduce transmission of malaria.
A total of 80 countries have officially adopted ACTs as their first line of treatment. Although 13 of these countries are not yet implementing this approach, most are deploying the medicines to a variable extent.
Plasmodium vivax malaria, which is the second most common type of malaria, also responds well to most ACTs. However, many countries continue to use chloroquine for its treatment because in most situations chloroquine is still effective against this parasite.
WHO has urged pharmaceutical companies to stop marketing oral artemisinin-based medicines as monotherapies, which may promote artemisinin resistance. WHO recommends that companies market ACTs only.
Pregnant women please note: Malaria chemoprophylaxis is not contraindicated in pregnancy. These drugs are usually well tolerated for pregnant women and children. However, due to prevalence of Cholroquine and SP resistance in most countries of the South East Asian region, these drugs would not guarantee full protection. Therefore, personal protection is strongly recommended.
All that you need to know about Malaria
How to prevent malaria?
There are three main ways to prevent malaria:
a) Prevent mosquito bites:
- Sleep under mosquito nets (ordinary or insecticide-treated): Malaria-transmitting mosquitoes usually bite from sunset to sunrise, so a mosquito net can prevent children and adults from mosquito bites while they sleep. Mosquito nets treated with special insecticide provide better protection. Make sure that mosquito nets are used correctly, and are in good condition.
- Screen all windows and doors in the house or, at least, in rooms where people sleep: A mosquito net only provides protection to those while sleeping under it. But screening a whole house can protect everyone living in it, because screening can prevent mosquitoes from entering the house. All windows and doors must be screened. All screens must be properly maintained to ensure that mosquitoes cannot enter.
- Apply mosquito repellents to the skin: Repellents are chemicals that are applied to the skin to keep mosquitoes away. They are readily available at chemists and pharmacies in all countries. They are effective when people are not using mosquito nets or are outside the house.
- Use mosquito coils: The smoke from mosquito coils keeps mosquitoes away, and may even kill them. They are useful when sitting outdoors, or in rooms that do not have screens.
b) Control mosquito breeding:
- Eliminate places where mosquitoes can lay eggs;
- Reclaim land by filling and draining;
- Introduce special fish that eat mosquito larvae; and
- Put special insecticides in the water to kill mosquito larvae.
c) Kill adult mosquitoes:
- Spray rooms with insecticides before going to bed; and
- Participate in activities carried out by the health services, such as spraying the inside walls of houses with insecticides that kill mosquitoes.
All that you need to know about Malaria
Where do mosquitoes breed?
Malaria mosquitoes may breed in:
- Fresh or brackish water (slightly salty) water, especially if it is stagnant or slow- flowing
- Open streams with very slow-flowing water along their banks
- Pools of water left after the rains or as a result of poor water management
- Swamps, rice fields, and reservoirs
- Small ponds, pools, borrow-pits, canals, and ditches with stagnant water, in and around villages
- Animal hoof-prints filled with water
- Cisterns (water tanks) for storage of water
- And anything that may collect water -- plant pots, old car tyres, etc. Mosquitoes usually 'operate' within a 2-kilometre radius.
All that you need to know about Malaria
What to do when someone has malaria?
Urgent treatment is needed at a clinic or hospital to save the patient's life. Do not waste any time in seeking good medical advice.
Remember, malaria is dangerous. But it is preventable through a multi-sectoral effort to address and control the problem by individuals, community, media and their sectors.
What is the role of the community and the individual?
While governments and NGOs can do a lot to control malaria, other sectors, such as the media, organised groups, communities and individuals, can play a more critical role in addressing the problem:
Governments must combat malaria through effective strategies and programmes. They must mount vast IEC campaigns to educate people about malaria, its spread and control. They can spray insecticides; and they can control mosquito breeding by reclaiming land and filling drains. They can anticipate and be prepared for epidemics.
NGOs can support governments in all of the above activities by disseminating information, and exercising vigilance to ensure that all precautions are taken.
Media can play its part by highlighting the dangers of malaria and the simple means to prevent it.
Communities and individuals can make sure they keep their surroundings safe by eliminating breeding grounds and stagnant water. They can keep their families safe by making them understand how malaria is spread. They can help by recognising the signs and symptoms and facilitating early diagnosis and treatment.




article